by Dr. Jeremy Selley
Reprinted with permission from Dr. Selley and The American College of Osteopathic Emergency Physicians (ACOEP). View the original article published in The Pulse, Summer 2023 by clicking here.
ED providers are so alike. We work very hard taking care of too many patients. We often spend more time coordinating social non-emergent issues than patients’ physical issues. Our workload is HUGE, our support and self-care suffer.
I have learned to welcome the break from the chaos of the ED. I was introduced to international medicine in 2016 when my wife and a local nurse in North Carolina decided that I would join her mission team to Honduras. Being voluntold can end in disaster, but in this instance, it was quite the opposite. I could have never guessed that my introduction to the Carolina Honduras Health Foundation (CHHF) would become my new passion.
I had always wanted to do some medical mission work, but years went by before opportunity met great timing. I had seen our local church take religious trips across the globe and watched medical teams help in Haiti and Guatemala. Unfortunately, I always found just the right excuse not to sign up. There was never anyone going on a trip that I knew… it wasn’t the right time… I’d be gone too long… the fee seemed too much. Isn’t it easy to find reasons to avoid something that is appealing but scary?
In July 2017, I finally took the leap and made my first trip to Honduras. I was nervous. It wasn’t my first time out of the country with a passport, but it was my first time on a medical mission to a third world country. I had no idea what to expect. I had served in the US Navy and had even went to Jordan, Kuwait, Dubai and Bahrain. I could not pinpoint why Honduras made me nervous, but it did. I even wrote a goodbye note to my wife and kids and placed it in the gun safe before leaving!
Once I arrived, thing appeared just simple. My journey became more about experiencing the beautiful culture of the country and less about my fears.
I found everything to be scaled down and less affluent. The people were all very friendly and welcoming. In some of the more populated areas I found a shanty next to a brand-new Pizza Hut. Many simple block homes did not have stucco, but the windows had bars and razor wire on top of their fences.
The trip from the airport in San Pedro Sula to the clinic in Limón took a full day. Two half days of driving with a one-night sleepover in La Ceiba where I was first introduced to Honduran fruit. The fruit. I could talk about it for hours (and crave it every day)! The fruit is absolutely amazing. Pineapple from Honduras is on a different level. Coupled with fresh coconut juice, that pineapple can make one hell of a Piña Colada. The fruit and fajitas that we had at the hotel the first night are truly what foodie dreams are made of. Once at the clinic in Limón, after settling into our rooms, we all gathered onto the porch. Lined with weather beaten wood rocking chairs, overlooking the ocean through dozens of coconut palms trees, there was an aura of solitude. It was such a contrast from the chaos I had expected to find.

The CHHF staff greeted us and we were introduced to Bexa and Elda, the two local cooks that would make us our food over the next 5 days, helping to cement my love for Honduran food and coffee. Both only speak Spanish, but the language of good food transcends any language barrier. It also provides the needed energy to face the long, busy days of clinics I was about to experience.
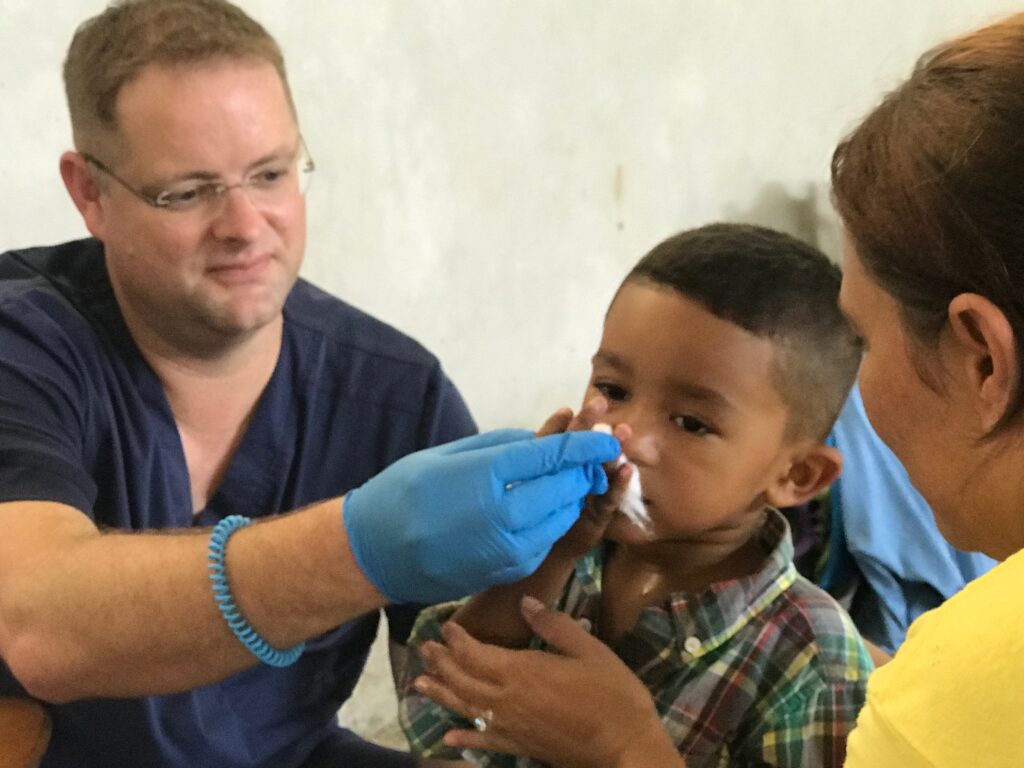
During four days of clinics, our team of 13 provided primary care to over 400 patients at the main clinic and two clinics in remote locations. The need for medical care was great, but there was such a huge difference from patients I typically saw in the ED. The patients I saw, many walking miles for their visit, were happy to see me. Every single one was happy, gracious, and thankful. When was the last time you were able to say that about a week of patient care?
Remote villages were an exciting part of the experience. Just getting there on an old yellow school bus on unpaved, rocky roads was interesting. The dust was overwhelming at times. At one point we were forced to push past a heard of cows to continue our drive. It’s certainly a reminder that we are not in the United States.
The children were so happy and playful. They comprised about 50% of the patients seen during the week. One young boy really touched my heart. Darlin was a 4-year-old who could barely walk the day I met him. He sustained a traumatic brain injury from an auto accident in 2017. He needed to see a neurosurgeon in San Pedro to have a skull plate placed to cover his brain. He needed to have his eye muscles corrected to fix his strabismus and he needed physical and occupational rehab. Without. His parents did not know where to begin. They also did not have the money to provide for this medical care. It was heartbreaking.

CHHF helps to coordinate and pay for referral specialist care for patients similar to Darlin that come to our clinic. Watching a young girl receive a leg prosthesis and walk for the first time, post traumatic leg amputation, with teams of joy streaming down her face, erasing two years of depression, is another example.
The villages served by the mission team are almost two hours from a hospital that does not even provide linen sheets or medication. If a patient finds transportation, they don’t the financial resources to pay. No one in Honduras goes to the ED for small issues like patients do in the USA.
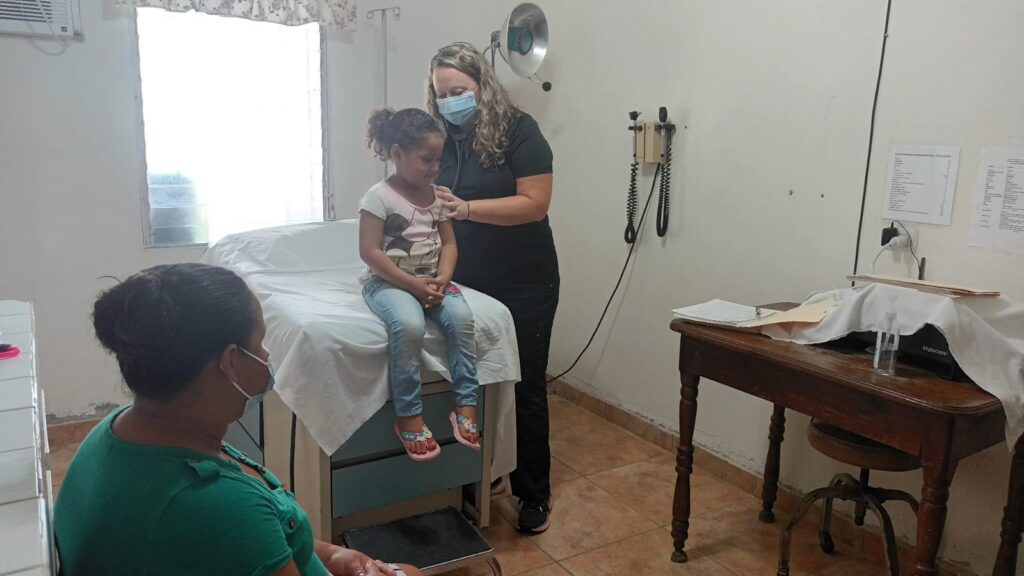
During my week, I saw a lot of kids with sniffles and coughs. There were adults with chronic HTN and DM. Unlike at the government clinics and hospitals in Honduras, all CHHF clinics provide medications for free. The teams pay for and bring what they will use with them, and then some. There is always an ongoing and revolving pharmacy supply of a full formulary that CHHF coordinates.
After the clinic days we reverse and make the 2-day trek back to the airport, sometimes with a day to decompress before making the long journey home. Uniformly, on the plane ride home, everyone starts to plan their trip for the following year, hoping they can make their schedule work. Before your feet touch the ground, you miss everything about Honduras. Because at this point, you have fallen in love with the country, people, food and most importantly the mission!
If you are like my wife, you sometimes just sit on the plane home, tearful, as the emotions overwhelm you and as you recant what an amazing experience from both a clinical and humanistic side. A medical mission team experience is difficult to explain, but it will change your life forever.
Dr. Jeremy Selley
My wife, my friends, and I are proof that you can fall in love with missions. As an added bonus, you have created new friends on your team, have new CHHF staff family members in Honduras, and have lasting memories, group chats and Facebook friends to last the rest of your life!
CHHF medical mission teams go 18 times a year. There is always room for you. Put the stress of working in the ED aside for one solid week. Serve under resourced villages full of people who are generous and grateful.
For more information, you can visit www.chhf.org or email us at contact@chhf.org. Take the first step and inquire today. I promise it will renew your spirit and refresh your energy.
About Dr. Selley
Jeremy Selley, DO, FACCEP, is a native of Nibley, Utah. He graduated from Utah State University with a B.S. and then went to Kirksville College of Osteopathic Medine for his D.O. Jeremy met his wife, Victoria H. Selley, D.O., in medical school and they then attended Emergency Medicine Residency at Lehigh Valley Health Network. After residency, Dr. Selley served 4 years in the US Navy and was deployed on the 24th Marine Expeditionary Unit in 2012. In 2014, Dr. Selley joined USADS full time and has been with the company since. In 2018, Drs. Selley moved from NC to FL and started work with AdventHealth Seabring. Dr. Selley began working with Carolina Honduras Health Foundation in 2017 and serves on their Board of Directors. He travels to Honduras yearly to help treat patients. Dr. Selley chairs the ACOEP Practice Advocacy Committee and works with Florida College of Emergency Physicians to increase advocacy awareness.
